As the founder, president and senior clinical director of Arm Dynamics, John has dedicated his career to positively transforming prosthetic rehabilitation for people with upper limb loss. He innovated a model of care that places each patient at the center of a multidisciplinary team of experienced upper limb prosthetists, occupational and physical therapists, technicians and insurance reimbursement specialists. The team provides holistic patient assessments, expedited prosthetic fitting and individualized prosthetic training, enabling patients to achieve dramatic and measurable improvements in comfort, wear time and functional ability. John’s advanced socket designs for all levels of upper limb loss have allowed Arm Dynamics to leverage emerging technologies to achieve optimal patient outcomes that were not possible with previous socket designs. His expertise in upper limb prosthetics and involvement in a range of international research projects led to the company’s appointment as a sole source provider of upper limb prosthetic services at Walter Reed National Military Medical Center, 2003-2014.
John is a Distinguished Fellow of the American Academy of Orthotists and Prosthetists (FAAOP-D) and received the AAOP Clinical Creativity Award in 2017. He completed his undergraduate studies at the University of Southern California and received his prosthetics certificate from Northwestern University. He is engaged in a range of research and development initiatives with the Department of Defense, DARPA, FDA, Cleveland Clinic, and prosthetic component designers and manufacturers around the world. He is recognized internationally for his presentations and publications on innovative care techniques, interface designs, prosthetic care for military amputees, and novel outcome measure assessments for people with upper limb loss.

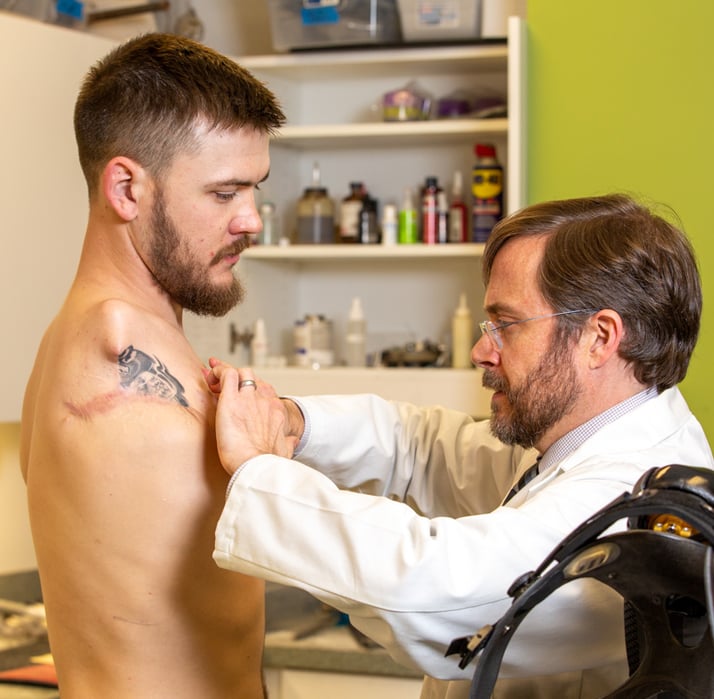



%20President%20and%20Senior%20Clinical%20Director.jpg?width=600&height=600&name=John%20M.%20Miguelez%2c%20CP%2c%20FAAOP(D)%20President%20and%20Senior%20Clinical%20Director.jpg)










